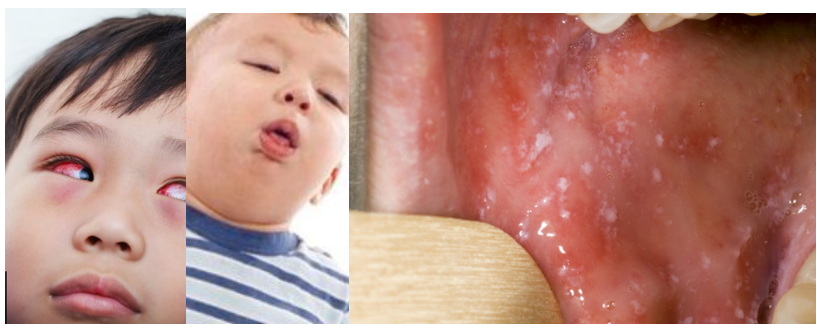
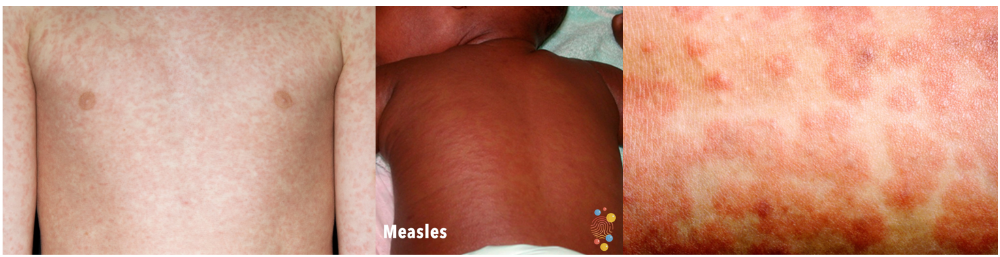
What should you do ?
If you think your child has measles, let your GP practice know.
● Measles usually starts to get better in about a week.
● To make your child more comfortable, you may want to lower their temperature using paracetamol (calpol) or ibuprofen.
If you've given your child one of these medications and they're still uncomfortable 2 hours later, you
could try the other medication. If this works, you can alternate paracetamol
and ibuprofen (every 2 to 3 hours), giving only 1 medicine at a time. Do not
give more than the maximum daily dose of either medicine.
● However, remember that fever is a normal response that may help the body to
fight infection. Paracetamol and ibuprofen will not get rid of it entirely.
Paracetamol and Ibuprofen bring down the temperature but do not treat the
infection. Whilst your child is unwell they will continue to get temperatures
once the effects of the medicine has worn off.
● Avoid sponging your child. It doesn’t actually reduce your child’s temperature
and may make your child shiver.
● Encourage your child to drink lots of fluids.
● If there are any crusts on your child's eyes, gently clean them using cotton
wool soaked in warm water.
● Your child can spread the infection to others from the time their symptoms
start until about 4 days after the rash appears.
● Children cannot go back to school or nursery until 4 days after the rash has
started. They should also avoid contact with babies, pregnant women, people
who have not had 2 doses of the MMR vaccine and people with weak immune
systems.
● If you are pregnant and haven't received 2 doses of the MMR vaccine, or if
there are any children in your family who are under 12 months old or any child
who hasn't had 2 doses of the MMR vaccine, please inform your GP practice
urgently. They might need immediate treatment to protect them from getting
measles.
● If your child with measles has been in contact with someone who has a very
weak immune system, let that person know about your child's measles. Ask
them to contact their GP practice or NHS Wales 111 urgently.
● Finally, make sure that you and your partner are up to date with your MMR
vaccines before getting pregnant. Measles can be extremely severe during
pregnancy and can harm your unborn baby.