Pain relief during labour
Give some thought to the kind of pain relief you want in labour. It's also helpful for whoever is going to be with you during your labour to know about the different options, as well as how they can support you.
Ask your midwife or doctor to explain what's available so you can decide what's best for you.
Write down your wishes in your birth plan, but remember you need to keep an open mind. You may find you want more pain relief than you'd planned, or your doctor or midwife may suggest more effective pain relief to help the delivery. Click here for advice on making a birth plan.
Even if you’re sure you want pain relieving drugs to help you cope with labour, it’s a good idea to find out what other help there is. In the early stage of labour, it’s usually best to try to avoid drugs.
You're likely to feel more relaxed in labour and better placed to cope with the pain if you:
- Learn about labour: this can make you feel more in control and less frightened about what's going to happen. Talk to your midwife or doctor, ask them questions and go to antenatal classes
- Keep moving: your position can make a difference, so try kneeling, walking around or rocking backwards and forwards. Click here for advice on different positions in labour and birth
- Bring a partner, friend or relative to support you during labour, but don't worry if you don't have one, your midwife will give you all the support you need
- Ask your partner to massage you (although you may find that you don't want to be touched)
Pain relief (without drugs)
Most antenatal classes teach breathing awareness as a way of coping with the pain of contractions. If you haven’t been to classes, talk to your midwife about breathing techniques for labour – she can quickly show you how to do it. The emphasis is on using breathing to help you stay relaxed, which helps you cope with the pain. Relaxation doesn’t take away pain, but it can prevent it from becoming stronger because tension increases pain levels. Research shows that when women are relaxed they release endorphins, the body’s own pain relievers.
Hypnobirthing is a method of pain management that can be used during labour and birth. It involves using a mixture of visualisation, relaxation and deep breathing techniques. Please click here for further information on hypnobirthing and a video on ‘How can I use breathing exercises during labour?’ from NHS Choices.

Most antenatal classes teach breathing awareness as a way of coping with the pain of contractions. If you haven’t been to classes, talk to your midwife about breathing techniques for labour – she can quickly show you how to do it. The emphasis is on using breathing to help you stay relaxed, which helps you cope with the pain. Relaxation doesn’t take away pain, but it can prevent it from becoming stronger because tension increases pain levels. Research shows that when women are relaxed they release endorphins, the body’s own pain relievers.
Hypnobirthing is a method of pain management that can be used during labour and birth. It involves using a mixture of visualisation, relaxation and deep breathing techniques. Please click here for further information on hypnobirthing and a video on ‘How can I use breathing exercises during labour?’ from NHS Choices.

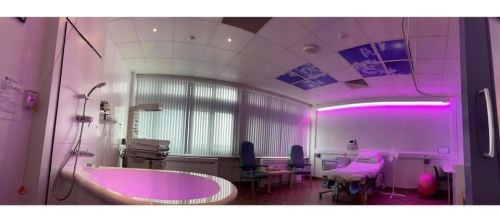
Water is very good at helping you to relax and make the contractions seem less painful. The water will be kept at a comfortable temperature, but not above 37.5C, and your temperature will be monitored. There are birthing pools in all of our Birth Centres and Birth Units.
The National Childbirth Trust has information on using water during labour and birth.
Water is very good at helping you to relax and make the contractions seem less painful. The water will be kept at a comfortable temperature, but not above 37.5C, and your temperature will be monitored. There are birthing pools in all of our Birth Centres and Birth Units.
The National Childbirth Trust has information on using water during labour and birth.

TENS – short for ‘transcutaneous electrical nerve stimulation’ is a form of pain relief provided by pads which fix to your back and which give a slight electrical charge. It can be effective in relieving pain and it is safe for you and your baby. It probably works best in the early stages of labour when many mums have lower back pain. If you want to try this, ask your midwife where you can hire or borrow a TENS machine.

TENS – short for ‘transcutaneous electrical nerve stimulation’ is a form of pain relief provided by pads which fix to your back and which give a slight electrical charge. It can be effective in relieving pain and it is safe for you and your baby. It probably works best in the early stages of labour when many mums have lower back pain. If you want to try this, ask your midwife where you can hire or borrow a TENS machine.

Complementary therapies such as homeopathy, hypnosis, acupuncture or acupressure can help some mums in labour. You will need to see a specialised practitioner if you are interested in these methods.

Complementary therapies such as homeopathy, hypnosis, acupuncture or acupressure can help some mums in labour. You will need to see a specialised practitioner if you are interested in these methods.

Pain relief (drugs)
‘Gas’, or ‘gas and air’, is a form of pain relief that is available in hospital and at home births. The gas comes with a tube and a mask or mouthpiece that you can breathe through when you need it, usually at the start of a contraction. It can take the ‘edge’ off the peak of the pain. The pain relief does not last very long and for it to work effectively you need to begin breathing it at the very start of the contraction so it builds up by the time the contraction is strongest. There is no danger of taking too much, but it can make some people feel sick. You can use gas with other kinds of pain relief. Babies do not appear to be affected by gas.

‘Gas’, or ‘gas and air’, is a form of pain relief that is available in hospital and at home births. The gas comes with a tube and a mask or mouthpiece that you can breathe through when you need it, usually at the start of a contraction. It can take the ‘edge’ off the peak of the pain. The pain relief does not last very long and for it to work effectively you need to begin breathing it at the very start of the contraction so it builds up by the time the contraction is strongest. There is no danger of taking too much, but it can make some people feel sick. You can use gas with other kinds of pain relief. Babies do not appear to be affected by gas.

This is an injection of a medicine called pethidine into your thigh or buttock to relieve pain. It can also help you to relax. Sometimes, less commonly, a medicine called diamorphine is used.
It takes about 20 minutes to work after the injection. You may feel sleepy and slightly ‘out of it’, so they cannot be used if you are in a birthing pool. Some women like this feeling and it helps them cope. Some don’t and feel out of control. Some women feel sick with these drugs and an anti–sickness medicine is usually given at the same time. The effects last between 2 and 4 hours, so would not be recommended if you're getting close to the pushing (second) stage of labour. If pethidine or diamorphine are given too close to the time of delivery, they may affect your baby's breathing, if this happens, another medicine to reverse the effect will be given. If you have had If pethidine or diamorphine in labour your baby may be sleepier and less interested in feeding, you will get extra help with feeding if you and your baby need it.
This is an injection of a medicine called pethidine into your thigh or buttock to relieve pain. It can also help you to relax. Sometimes, less commonly, a medicine called diamorphine is used.
It takes about 20 minutes to work after the injection. You may feel sleepy and slightly ‘out of it’, so they cannot be used if you are in a birthing pool. Some women like this feeling and it helps them cope. Some don’t and feel out of control. Some women feel sick with these drugs and an anti–sickness medicine is usually given at the same time. The effects last between 2 and 4 hours, so would not be recommended if you're getting close to the pushing (second) stage of labour. If pethidine or diamorphine are given too close to the time of delivery, they may affect your baby's breathing, if this happens, another medicine to reverse the effect will be given. If you have had If pethidine or diamorphine in labour your baby may be sleepier and less interested in feeding, you will get extra help with feeding if you and your baby need it.
An epidural is when pain–relieving drugs are injected into the space around your spinal nerves. The aim of the epidural is to relieve the pain of labour by reducing the sensation in your lower body. You will still be able to move around the bed and push when giving birth. An epidural is the most effective form of pain relief in labour. It is especially useful if your labour is long or complicated and if your baby needs close monitoring. An epidural can only be given to you by an anaesthetist, so it is not available at every unit.
Side effects
An epidural does not cause you to be sleepy. Sometimes your legs might feel numb or heavy which can make it harder to push. This means it can increase the risk of needing help with the birth, like a ventouse or forceps delivery. It does not increase your risk of a caesarean section. The numbness can last up to a few hours after the delivery. Sometimes an epidural can make your baby a bit sleepy after birth and make learning to breastfeed more difficult. Occasionally an epidural can give mums a bad headache for some days after the birth and mild itching is also possible

An epidural is when pain–relieving drugs are injected into the space around your spinal nerves. The aim of the epidural is to relieve the pain of labour by reducing the sensation in your lower body. You will still be able to move around the bed and push when giving birth. An epidural is the most effective form of pain relief in labour. It is especially useful if your labour is long or complicated and if your baby needs close monitoring. An epidural can only be given to you by an anaesthetist, so it is not available at every unit.
Side effects
An epidural does not cause you to be sleepy. Sometimes your legs might feel numb or heavy which can make it harder to push. This means it can increase the risk of needing help with the birth, like a ventouse or forceps delivery. It does not increase your risk of a caesarean section. The numbness can last up to a few hours after the delivery. Sometimes an epidural can make your baby a bit sleepy after birth and make learning to breastfeed more difficult. Occasionally an epidural can give mums a bad headache for some days after the birth and mild itching is also possible

What is remifentanil PCA?
Remifentanil is a very short-acting pain relieving drug rather like pethidine. Its pain relieving effect comes on very rapidly, and also wears off very quickly afterwards. A small dose of the remifentanil is given into a drip in your arm at your request by pushing a button on an electronic pump.
Who can use remifentanil?
Any woman in labour can request to use remifentanil PCA. We would advise women with an allergy to morphine, pethidine or other related drugs not to use remifentanil. Remifentanil may be useful also in certain situations where a woman cannot have or does not want an epidural. If you try remifentanil and then decide to change to another method of pain relief in labour (e.g. pethidine, epidural), all the other options for pain relief are open to you. Having tried remifentanil does not limit your choice.
How is it given?
To use remifentanil you will need to have a cannula (“drip”) placed in a vein, usually on the back of your hand or arm. Otherwise, you need no extra treatment or drugs given. You do not need a catheter in the bladder. The drip is connected to an electronic pump, which delivers a small dose of the drug once you press the hand-held button. The pain-relieving effect is felt usually in 20 to 30 seconds, and wears off again within a few minutes. You are in control and you get the drug when you need it and not in between contractions. There is a safety feature built into the pump so that you can only get a safe amount of the drug. You can use the pump at any time right up to your delivery if you wish, and the effects will still wear off very quickly when you stop using the pump after your baby has been born.
Are there any unwanted effects of remifentanil?
Some women can get sleepy between contractions, as tends to happen also with pethidine. However, even if you are drowsy, this will wear off very quickly after you stop using the pain relief. As part of our routine observations with remifentanil your midwife will measure your oxygen level using a sensor (like a peg) on your finger, as well as your level of pain relief and drowsiness at regular intervals. Otherwise all observations and treatment is the same as for any other woman on labour ward. Remifentanil has been shown to be safe for babies. Other unwanted effects can be nausea, vomiting and itch. These are also side-effects of pethidine.
When can I ask for remifentanil?
You can request remifentanil at any time in your labour. Your midwife will contact the anaesthetist, who will confirm your suitability, answer any questions you may have, and then set up the syringe and pump
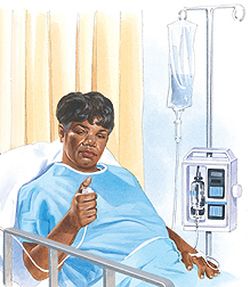
What is remifentanil PCA?
Remifentanil is a very short-acting pain relieving drug rather like pethidine. Its pain relieving effect comes on very rapidly, and also wears off very quickly afterwards. A small dose of the remifentanil is given into a drip in your arm at your request by pushing a button on an electronic pump.
Who can use remifentanil?
Any woman in labour can request to use remifentanil PCA. We would advise women with an allergy to morphine, pethidine or other related drugs not to use remifentanil. Remifentanil may be useful also in certain situations where a woman cannot have or does not want an epidural. If you try remifentanil and then decide to change to another method of pain relief in labour (e.g. pethidine, epidural), all the other options for pain relief are open to you. Having tried remifentanil does not limit your choice.
How is it given?
To use remifentanil you will need to have a cannula (“drip”) placed in a vein, usually on the back of your hand or arm. Otherwise, you need no extra treatment or drugs given. You do not need a catheter in the bladder. The drip is connected to an electronic pump, which delivers a small dose of the drug once you press the hand-held button. The pain-relieving effect is felt usually in 20 to 30 seconds, and wears off again within a few minutes. You are in control and you get the drug when you need it and not in between contractions. There is a safety feature built into the pump so that you can only get a safe amount of the drug. You can use the pump at any time right up to your delivery if you wish, and the effects will still wear off very quickly when you stop using the pump after your baby has been born.
Are there any unwanted effects of remifentanil?
Some women can get sleepy between contractions, as tends to happen also with pethidine. However, even if you are drowsy, this will wear off very quickly after you stop using the pain relief. As part of our routine observations with remifentanil your midwife will measure your oxygen level using a sensor (like a peg) on your finger, as well as your level of pain relief and drowsiness at regular intervals. Otherwise all observations and treatment is the same as for any other woman on labour ward. Remifentanil has been shown to be safe for babies. Other unwanted effects can be nausea, vomiting and itch. These are also side-effects of pethidine.
When can I ask for remifentanil?
You can request remifentanil at any time in your labour. Your midwife will contact the anaesthetist, who will confirm your suitability, answer any questions you may have, and then set up the syringe and pump

Video: what pain relief will be available in labour?
In this NHS video, a midwife outlines what pain relief options there are during labour.
LabourPains website committee which is part of the Obstetric Anaesthetists Association, supported by The Royal College of Midwives, has additional information on pain relief and anaesthetic choices for your baby’s birth. https://www.labourpains.com/home
Many women choose to have pain relief in labour. This is an information film designed to guide you step by step through the process of having an epidural, answering key questions about what is involved, and is based on the information leaflet developed by the the LabourPains website.




