When your baby is nearly ready to be born
For most mums the hardest part of labour is towards the end of the first stage, just before the pushing begins. Your contractions will be very strong and you will not have much time in between them to catch your breath and relax. This part is often called transition.
Transition: what you can expect
Transition affects how you feel emotionally as well as physically. You may feel impatient, tired, irritable and even angry and frustrated with the people looking after you. This is a perfectly natural reaction and it means that the birth of your baby is not far off.
- Try to remember that although it’s hard, it’s normal and your baby is nearly here
- Make the most of the space that there is between contractions and completely relax – ignore everyone else
For birth partners
Don’t take her behaviour personally, nothing you do will be right! It’s perfectly normal and is usually a good sign that the baby is nearly here.
The second stage
This is the stage where your baby arrives. It begins when the neck of your womb (your cervix) is fully open (to 10 centimetres) and ends with the birth of your baby. With a first baby this stage can last anywhere between ten minutes and two hours, or sometimes even longer. It’s usually easier and shorter with your second baby.
Positions for birth
There’s no right or wrong position for you to give birth in. However, lying on your back is usually uncomfortable and makes it more difficult to push your baby through your pelvis, so it is not recommended. When women are encouraged to do what feels best, they hardly ever adopt this position. If possible, get gravity to help you and stay upright and active.
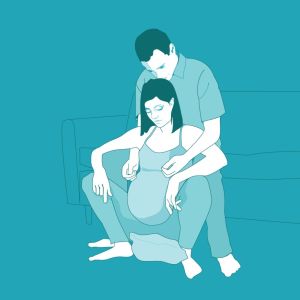
Supported standing or squatting
This position is good for the birth, it allows your pelvis to open wide and your baby to be born with the help of gravity. You will need support for your upper body to keep your balance. Your partner can support you from behind by holding you under your arms, though they will need the strength to take all of your weight and may find sitting in a chair makes this easier
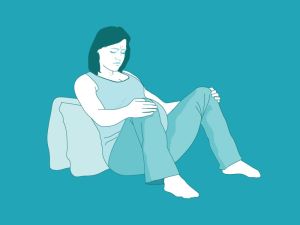
All fours
This position also allows your pelvis to open wide and can feel very safe and steady as you are supported by all your arms and legs. You can sit back on your heels and take a breather and a sip of water in between contractions.
Supported kneel
A supported kneel will open your pelvis wider than sitting or lying down, while allowing your body to be completely supported.
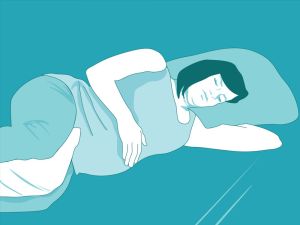
Leaning on the back of the bed
If you are on the bed this is a great position, it gives your pelvis freedom to open and you have something to lean on. This is a good position if your baby’s heart beat needs to be continuously monitored.
Pushing can be hard work with your first baby and it can take a little while to get the hang of what you’re doing. Your midwife will help you listen to your body and focus your energy so your pushes are effective if you need her to.
The birth of your baby
Most babies come into the world head first, so it is your baby’s head that will stretch the birth canal when your baby is very nearly born
The muscle and skin at the opening to your vagina will start to stretch and this can produce a stinging or burning sensation. At this stage your midwife may ask you not to push, or only give tiny pushes to slow things down to give you time to stretch. Very occasionally if the stretching is taking a while and your baby needs to be born quickly, the midwife (with your permission) will give this bit of skin and muscle a small cut. You will have an injection so you do not feel this – and it will all be explained to you. This cut is called an episiotomy.
For your birth partner
This stage is very intense and you can really help your partner if you:
- Keep calm and tell her how well she is doing
- Help her be as comfortable as possible
- Don’t talk too much and make sure she can really relax in between contractions
- Think about where you want to be when the baby is born. Do you want to see your baby being born, or would you rather support your partner and greet the baby later?
Every birth is unique and special, it may not have been the birth you have anticipated but you will usually remember it as one of the most important moments of your life.
If you and your baby need help
Sometimes you or your baby will need some help during labour. This could be because your baby is getting too stressed, or labour has been hard and long and you have no more strength left. If you need help before you are in the second ‘pushing’ stage, you will probably have an unplanned caesarean section. Once you are in the second stage your doctor or midwife may be able to help using forceps or ventouse.
If you need help with forceps or ventouse
Forceps and ventouse are both instruments that can be attached to your baby’s head so that the doctor or midwife can help you as you push. Forceps are made of metal and look a bit like large spoons for serving salad, a ventouse is made of soft plastic and is like a cup that fits on your baby’s head. You will be given a local anaesthetic – an injection to make the skin and muscle at the opening to your vagina numb and your bladder may be emptied by a thin tube inserted into your bladder – called a catheter and you will probably need a small cut (called an ‘episiotomy’) to allow room for the forceps or ventouse to be inserted. You will probably be helped to lie down on your back and your legs will be raised. Occasionally your baby will have a mark (bruising or swelling) from the forceps or ventouse cup on his head, but don’t worry it will soon fade.